How Is Chronic Leukaemia Treated? A Step-by-Step Guide
Chronic leukaemia is not a single, one-size-fits-all disease—and thankfully, its treatment isn’t either. Over the past two decades, advances in medical research have transformed how doctors manage this long-term blood cancer. Today, many patients live full, active lives for years after diagnosis.
So how is chronic leukaemia treated? Let’s break it down step by step, in plain English, without hype or fear-based language—just facts, context, and clarity.
Understanding Chronic Leukaemia
Before diving into treatment, it helps to understand what makes chronic leukaemia different from other blood cancers.
What Makes Leukaemia “Chronic”?
“Chronic” means the disease usually progresses slowly. Unlike acute leukaemia, which requires immediate treatment, chronic leukaemia may remain stable for months or even years before therapy is needed.
Common Types of Chronic Leukaemia
There are two main forms doctors commonly diagnose.
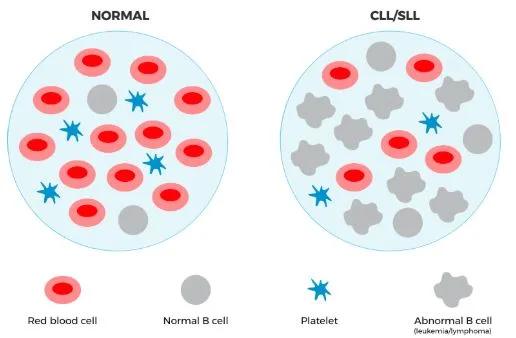
Chronic Lymphocytic Leukaemia (CLL): CLL affects lymphocytes, a type of white blood cell involved in immune defense. It’s the most common chronic leukaemia in adults.
Chronic Myeloid Leukaemia (CML): CML originates in myeloid cells and is often associated with a specific genetic change known as the Philadelphia chromosome.
Why Treatment Approaches Differ Between Patients
No two patients follow the exact same treatment path—and that’s intentional.
Disease Stage and Progression: Some people are diagnosed early with few symptoms. Others may already have signs such as anemia, infections, or enlarged lymph nodes. Treatment timing depends heavily on disease activity.
Patient Health and Age: Doctors also consider overall health, existing conditions, and how well a patient might tolerate certain therapies. Treatment decisions are personalized, not automatic.
Step 1: Diagnosis and Risk Assessment
Treatment starts with understanding the disease as precisely as possible.
Blood Tests and Bone Marrow Analysis: Routine blood work often reveals abnormal white blood cell counts. Bone marrow tests help confirm the diagnosis and measure disease burden.
Genetic and Molecular Testing: Modern testing looks for genetic markers that influence prognosis and guide therapy choices. These details matter more today than ever before.
Step 2: Watchful Waiting (Active Surveillance)
When Immediate Treatment Is Not Required: If symptoms are mild or absent, doctors may recommend close monitoring instead of immediate therapy. This approach avoids unnecessary side effects while keeping a careful eye on disease progression.
Step 3: First-Line Treatment Options
When treatment is needed, several options are available depending on disease type and patient factors.
Targeted Therapies: Targeted treatments focus on specific pathways that cancer cells rely on to survive.
Oral Targeted Medications: Many modern therapies are taken orally and work by interrupting signals that promote leukaemia cell growth. These treatments have reshaped expectations around chronic leukaemia treatment, offering more precise disease control with manageable side-effect profiles.
Chemotherapy and Immunotherapy: In some cases, chemotheray is combined with immunotherapy—medications that help the immune system recognize and attack cancer cells.
Step 4: Managing Side Effects and Monitoring
Treatment doesn’t end with the prescription, it continues with careful follow-up:
Common Side Effects: Fatigue, infections, and blood count changes are possible, depending on therapy type. Doctors adjust treatment plans as needed to maintain safety.
Ongoing Monitoring and Follow-Ups: Regular blood tests and checkups help ensure treatment remains effective and complications are addressed early.
Step 5: Treatment for Relapsed or Resistant Disease
Sometimes the disease stops responding to therapy. When that happens, there are still options.
Changing or Combining Therapies: Doctors may switch medications, combine treatments, or adjust doses to regain disease control.
The Role of Clinical Trials: Clinical research plays a crucial role in advancing care.
Why Clinical Research Matters: Clinical trials give patients access to emerging therapies while helping scientists improve future standards of care. Participation is always voluntary and carefully regulated.
Living With Chronic Leukaemia: Chronic leukaemia is often managed as a long-term condition.
Quality of Life and Long-Term Care: With ongoing monitoring, many patients maintain work, travel, and daily routines. Supportive care—including nutrition, mental health support, and physical activity—remains an important part of management.
What are the Latest Advances in Chronic Leukaemia Treatment?
Research continues to reshape expectations of the CLL treatment:
Precision Medicine and Targeted Approaches: As genetic testing improves, treatments are becoming more individualized, aiming to maximize effectiveness while minimizing unnecessary exposure.
Questions Patients Often Ask: Patients commonly wonder how long treatment lasts, whether therapy is lifelong, and how outcomes may change over time. These answers vary—but open communication with care teams helps set realistic expectations.
Key Takeaways
Chronic leukaemia treatment is no longer defined by urgency alone—it’s defined by precision, timing, and personalization. From careful diagnosis and watchful waiting to targeted therapies and long-term monitoring, each step is guided by evidence and patient-specific factors.
While a diagnosis can feel overwhelming, today’s step-by-step treatment approach allows many individuals to live well while managing the disease over time.
Frequently Asked Questions (FAQs)
1. Is chronic leukaemia always treated immediately?
No. Many patients are monitored for months or years before treatment becomes necessary.
2. Can chronic leukaemia be cured?
It is often managed as a long-term condition, with treatment aimed at controlling disease progression.
3. Are newer treatments less intensive than chemotherapy?
Many targeted therapies are more specific and may have different side-effect profiles compared to traditional chemotherapy.
4. How often do patients need follow-up visits?
Follow-up frequency depends on disease stage and treatment phase but typically involves regular blood tests.
5. Do all patients qualify for the same treatments?
No. Treatment decisions depend on genetics, disease behavior, and overall health.




